Spondylolisthesis (Degenerative) Symptoms & Treatment
Degenerative spondylolisthesis occurs when age-related disc and joint changes cause one vertebra to slip forward over another. It commonly affects older adults and may lead to lower back pain, stiffness, or leg symptoms. Treatment usually includes physical therapy, activity modification, pain management, and surgery only in severe cases.
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
Spondylolisthesis is a spinal condition in which one vertebra in the lower back slips forward over the vertebra beneath it. This forward movement is commonly caused by repeated stress on the joints of the lower spine and is often associated with age-related degenerative changes such as arthritis.
While spondylolisthesis can lead to low back pain, stiffness, and sciatica due to nerve compression, some individuals may experience little to no noticeable symptoms despite the presence of the condition.
What causes Spondylolisthesis (Degenerative)?
There are several causes of spondylolisthesis, classified into different types:
- Type 1 – Congenital: This type is present at birth and occurs due to a defect in one of the vertebrae, most commonly the L5 vertebra.
- Type 2 – Isthmic: This type usually develops in children and young adults and is caused by repeated stress or overuse of the lower back, leading to a small fracture or weakness in the vertebra.
- Type 3 – Degenerative: Degenerative spondylolisthesis develops later in life as an acquired condition. It results from chronic disc degeneration and wear of the spinal joints, leading to long-term lumbar instability and gradual vertebral slippage, most commonly at the L4–L5 level. This type is frequently seen in individuals with an aging spine.
How the Injury Occurs: Degenerative spondylolisthesis happens as the discs in the spine wear down over time. As the discs lose height and flexibility, more stress is placed on the joints and ligaments that support the spine. When these supports weaken, one vertebra can slowly slide forward over the one below it.
Common Everyday Causes
- Age-related wear and tear of spinal discs and joints
- Long-term poor posture
- Repetitive bending or twisting movements
- Prolonged standing or walking
- Weak core and back muscles
- Occupations or activities that place repeated stress on the lower back
Symptoms
The most common symptom of spondylolisthesis is low back pain.
Common symptoms also include:
- Pain in the lower back that feels like a muscle strain
- Pain that spreads to the buttocks and thighs
- Pain that gets worse with physical activity
Patients with a slipped vertebra (spondylolisthesis) may also experience tingling, numbness, or weakness due to pressure on nearby nerves.
When to see a doctor
You should see a doctor if you have persistent back pain that does not improve with conservative treatments. If you experience neurological symptoms such as numbness, tingling, or weakness in your legs, it is important to schedule an appointment with your physician promptly.
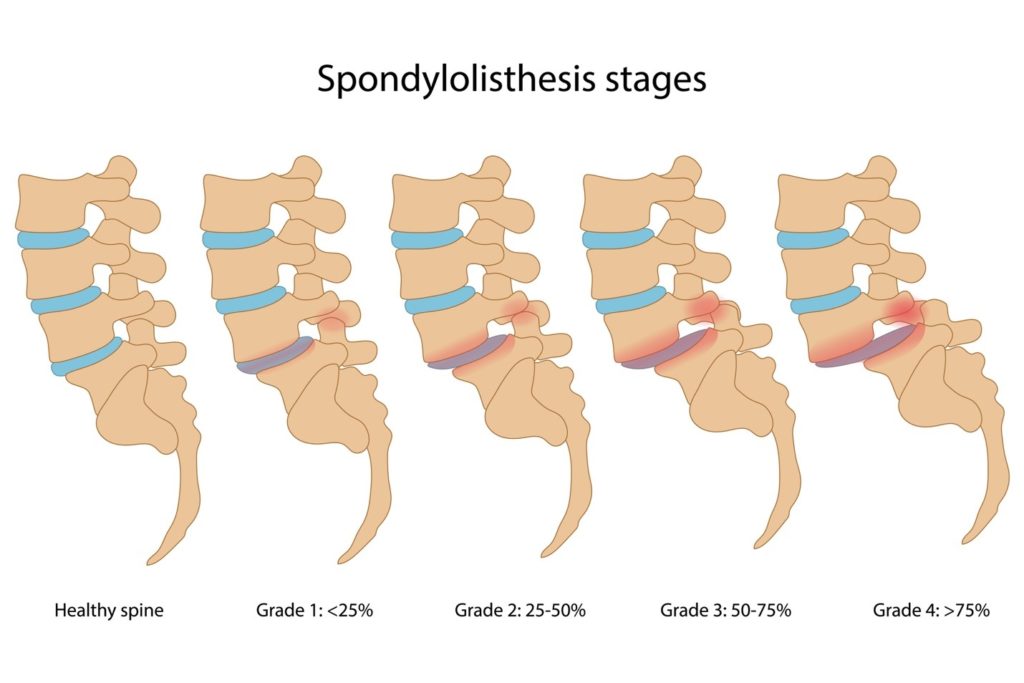
During a physical examination, your doctor will check for tenderness, assess your range of motion, and evaluate your posture and gait. X-rays or other imaging tests may be ordered to determine if there is a vertebral fracture or nerve involvement. Imaging also helps assess the degree of slippage, which is often classified as “low grade” or “high grade.”
Non-operative treatment
Non-operative treatment is usually effective for cases of low-grade spondylolisthesis. Examples of conservative spondylolisthesis treatment include:
- Rest from sports that place stress on the back
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, are used for pain relief
- Wearing a back brace to limit movement and promote healing of the muscles and bones of the lower back
- Physical therapy for muscle stretching and strengthening
Try these exercises to help address your condition:
Below is a PDF of the Exercise Program
Surgical Treatment
Your doctor may recommend a surgical procedure if you have a high-grade spondylolisthesis or if conservative measures such as physical therapy, medications, and lifestyle modifications are not effective in relieving your symptoms. Surgery is generally considered when there is significant vertebral slippage, persistent pain, nerve compression, or neurological symptoms.
The type of surgery typically involves decompression to relieve pressure on the nerves and spinal fusion to stabilize the affected vertebrae. Your doctor will evaluate your overall health, imaging results, and severity of symptoms to determine whether surgery is a suitable option for you.
Recovery
Recovery from spondylolisthesis depends on the grade of the condition and the type of treatment received. For low-grade spondylolisthesis, non-surgical treatments such as activity modification, physical therapy, and core strengthening exercises are often effective, leading to a relatively quick recovery.
Recovery following surgery is generally longer and can take up to six months. During this period, patients gradually regain strength, flexibility, and mobility while following a structured rehabilitation plan. Regular follow-ups with the doctor are important to monitor healing and ensure the spine remains stable.
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
Is surgery always required for spondylolisthesis?
In most cases, especially low-grade slips, respond well to non-operative treatments such as physical therapy, NSAIDs, and bracing. Surgery is typically considered only when symptoms persist despite conservative care.
How effective is physical therapy in managing symptoms?
Physical therapy is highly effective for many patients. It focuses on stretching tight muscles, strengthening the core, and improving spondylolisthesis posture, which helps stabilize the spine and relieve pressure on affected nerves.
What are the benefits of early diagnosis?
Early diagnosis allows for timely intervention with non-invasive strategies, potentially preventing the progression of the slip and avoiding surgery. It also helps patients make lifestyle adjustments that protect spinal health in the long term.
Can lifestyle changes help manage this condition?
Adopting a spine-friendly lifestyle—including low-impact exercise, ergonomic posture, weight management, and avoiding heavy lifting—can significantly reduce symptoms and improve mobility and comfort.

