Shoulder (Glenohumeral) Arthritis
Shoulder (glenohumeral) arthritis is a degenerative joint condition where cartilage in the shoulder wears down, causing pain, stiffness, and reduced range of motion. It can result from aging, injury, or overuse, making everyday movements like lifting or reaching increasingly difficult.
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
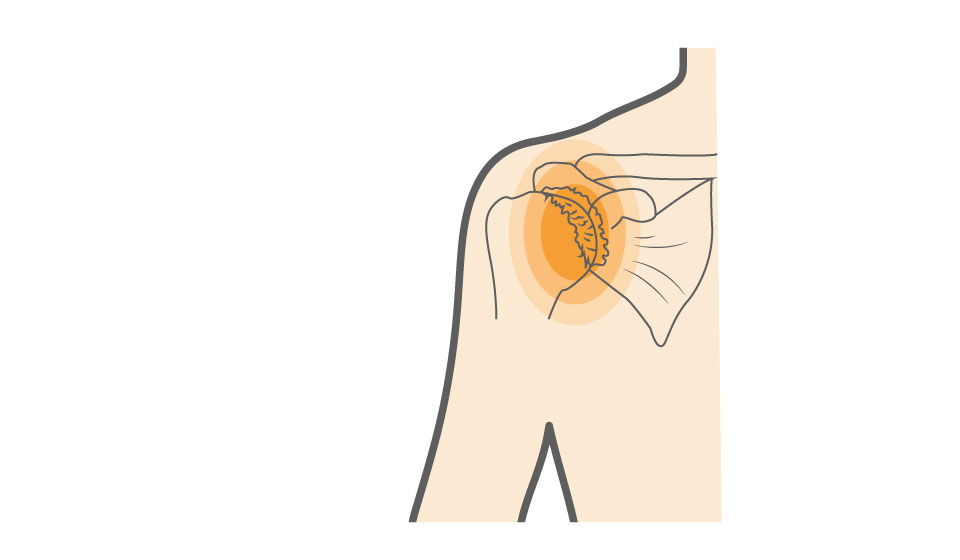
Shoulder joint arthritis, also known as glenohumeral joint arthritis, is a condition marked by damage to the cartilage within the shoulder joint. The glenohumeral joint is the main shoulder joint, where the head of the humerus (upper arm bone) fits into the glenoid cavity of the scapula (shoulder blade).
The ends of these bones are normally covered with smooth cartilage, which allows the joint to move easily and without friction. When this cartilage becomes damaged or worn away, the bones may rub against each other, leading to inflammation, grinding sensations, pain, and progressive joint damage.
Three types of arthritis in the shoulder joint affect the shoulder:
- Osteoarthritis: The most common form, caused by the gradual wear and tear of the joint cartilage due to aging.
- Rheumatoid arthritis: An autoimmune condition in which the body’s immune system attacks the joint lining, leading to joint degeneration.
- Post-traumatic arthritis: A type of osteoarthritis that develops after a shoulder injury damages the cartilage and alters normal joint mechanics, accelerating cartilage wear.
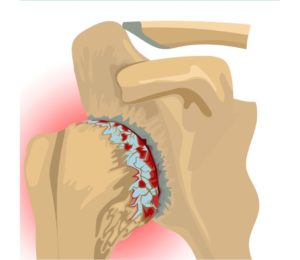
In all forms of shoulder arthritis, the cartilage covering the ends of the bones is gradually lost. Osteoarthritis remains the most common type affecting the shoulder.
What causes Shoulder (Glenohumeral) Arthritis?
The cause of shoulder arthritis depends on the specific type diagnosed, as each form affects the joint differently.
- Osteoarthritis: Develops from the gradual wear and tear of shoulder cartilage over time, commonly associated with aging.
- Rheumatoid arthritis: An autoimmune condition in which the immune system attacks the joint lining, leading to inflammation and cartilage damage.
- Post-traumatic arthritis: Occurs after a shoulder injury, such as a fracture or dislocation, that disrupts normal joint mechanics and accelerates cartilage breakdown.
How the Injury Occurs: Shoulder arthritis develops when repeated stress, inflammation, or injury causes the cartilage in the glenohumeral joint to gradually wear away.
Common Everyday Causes: Daily activities such as repetitive overhead reaching, lifting heavy objects, poor posture, and long-term occupational strain can contribute to cartilage breakdown and shoulder arthritis symptoms.
Shoulder arthritis is more common in individuals who play or have played these sports:
- Baseball: Repetitive throwing places high stress on the shoulder joint over time.
- Tennis: Frequent overhead swings and serving motions increase joint wear.
- Weightlifting: Heavy lifting and repeated shoulder loading can strain and damage joint cartilage.
- Football: Repeated impacts, tackles, and shoulder injuries contribute to long-term joint degeneration.
Symptoms
Pain in the shoulder is the most common and noticeable symptom of shoulder arthritis. Other symptoms may include:
- Shoulder stiffness: Reduced flexibility and difficulty moving the shoulder, especially after rest or inactivity.
- Clicking or grinding: Sensations or sounds caused by damaged cartilage and bone rubbing during movement.
- Weakness: Loss of shoulder strength, typically developing in more advanced stages of the condition.
When to see a doctor
If you have symptoms of shoulder arthritis that persist or continue to worsen, it is important to schedule an appointment with an orthopedic specialist. During the visit, your doctor will review your symptoms and perform a physical examination to evaluate shoulder strength and range of motion.
To confirm a diagnosis, your doctor may recommend the following imaging tests:
- X-rays: To assess joint space narrowing, bone changes, and signs of arthritis.
- MRI: To evaluate surrounding shoulder structures, especially the rotator cuff and soft tissues.
Non-operative treatment
Shoulder arthritis is usually managed first with conservative, non-surgical approaches, which aim to reduce arthritis shoulder pain and improve function. Common treatments include:
- Rest from aggravating activities: Avoiding movements that worsen pain helps prevent further joint irritation.
- Non-steroidal anti-inflammatory medications (NSAIDs): These relieve pain and reduce inflammation in the shoulder joint.
- Physical therapy: Targeted shoulder exercises strengthen surrounding muscles, improve mobility, and support joint stability.
- Cortisone injections: Administered to reduce inflammation and provide temporary pain relief in the affected joint.
Try these shoulder arthritis exercises to help address your condition:
Below is a PDF of the Exercise Program
Surgical Treatment
If non-operative treatments do not relieve your symptoms of shoulder arthritis, your doctor may recommend surgery. The type of surgery performed will depend on the severity of your diagnosis and your age.
- Debridement: During a debridement procedure, your doctor cleans out damaged cartilage from the shoulder joint. This procedure is recommended if you still have cartilage tissue and the bones are not rubbing against each other.
- Total Shoulder Replacement: The head of the humerus (upper arm bone) and the glenoid (socket) are replaced with artificial parts.This is the most common procedure performed for shoulder arthritis.
Recovery
Although there is no cure for shoulder arthritis, patients can find relief from symptoms using non-operative treatments. If non-surgical treatments are effective, you may find relief within a couple of weeks.
If you elect to have shoulder replacement surgery, you will need to keep your arm in a sling for several weeks to allow the shoulder to heal. When instructed by your doctor, you will start physical therapy to regain the range of motion and strength of the shoulder and arm.
Most shoulder surgeries require at least three months of healing and rehabilitation. If you undergo a total shoulder replacement, initial recovery typically takes three to six months, as the joint heals and daily function improves. Regaining full strength and range of motion, however, can take up to a year, depending on your activity level and commitment to physical therapy.
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
Can degenerative shoulder joint conditions be managed without surgery?
Many patients find relief through non-operative treatments like physical therapy, medication, and lifestyle changes that improve shoulder function and reduce symptoms such as shoulder grinding.
How can I tell if my shoulder grinding is related to arthritis?
Shoulder grinding accompanied by pain, stiffness, or limited motion often indicates cartilage damage from arthritis. Consulting a specialist early can help diagnose and manage the condition effectively.
What types of exercises help improve symptoms of shoulder arthritis?
Targeted shoulder arthritis exercises strengthen muscles around the joint, increase flexibility, and decrease pain, helping improve overall shoulder health and mobility.
Is recovery from shoulder replacement surgery successful for most patients?
Yes, with proper care and rehabilitation, most patients experience significant pain relief and improved shoulder function after recovery from surgery, enabling them to return to activities of daily living and some sports.

