Plantar Fasciitis
Plantar fasciitis is a common foot condition caused by inflammation of the plantar fascia, the thick band of tissue connecting the heel to the toes. It leads to sharp heel pain, especially with the first steps in the morning or after prolonged standing, and can affect daily walking and activities.
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
The plantar fascia acts as a natural shock absorber, helping the foot handle the daily impact, strain, and stress from walking, running, and jumping. In athletes, repetitive high-impact activities place extra stress on this ligament. Excessive strain can lead to small tears, inflammation, and heel pain, resulting in plantar fasciitis.
- How the Injury Occurs: Plantar fasciitis develops when repetitive stress or sudden increases in activity create micro-tears in the plantar fascia, leading to inflammation and pain in the heel.
- Common Everyday Causes: Daily activities such as prolonged standing, walking on hard surfaces, wearing unsupportive shoes, or carrying excess body weight can also contribute to plantar fascia strain and heel pain.
Athletes with the following risk factors are more likely to develop plantar fasciitis:
- Tight Achilles tendon: Reduced flexibility increases tension on the plantar fascia during movement.
- Tight calf muscles: Limited calf mobility forces extra strain on the foot’s arch.
- Wearing shoes that don’t provide enough arch support: Inadequate footwear fails to absorb shock and stabilize the foot, contributing to ligament stress.
Plantar fasciitis is most common in these sports:
- Baseball: Frequent running and sudden sprinting put repeated stress on the heel.
- Basketball: Jumping and quick directional changes overload the plantar fascia.
- Football: Explosive movements and hard surface play increase heel impact.
- Running: High mileage and repetitive heel strikes strain the ligament.
- Soccer: Sprinting, cutting, and kicking motions intensify foot stress.
- Lacrosse: Rapid running, twisting, and stopping add repeated strain on the plantar fascia.
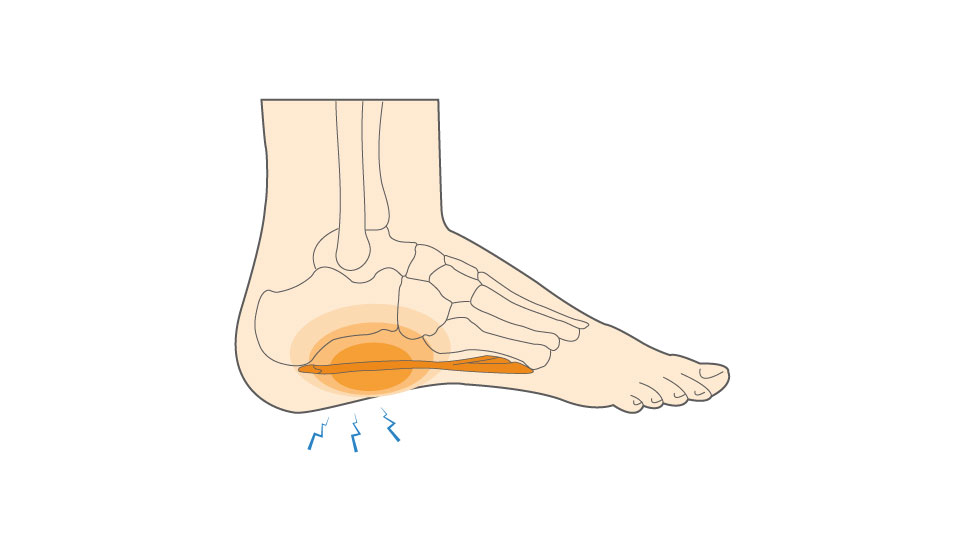
What causes Plantar Fasciitis?
The plantar fascia acts as a shock absorber for the impact, strain, and stress we put on our feet daily. This pressure is exaggerated for athletes, as the impact of running and jumping greatly stresses the ligament. When too much strain is placed on the plantar fascia, small tears can develop that become inflamed and cause heel pain. Athletes with the following risk factors are more likely to develop plantar fasciitis:
• Tight Achilles tendon
• Tight calf muscle
• Wearing shoes that don’t provide enough arch support
Plantar fasciitis is most common in these sports:
• Baseball
• Basketball
• Football
• Running
• Soccer
• Lacrosse
Symptoms
Plantar fasciitis typically causes pain on the bottom of the heel, which can range from a sharp sting to a dull, aching discomfort. Common situations that trigger heel pain include:
- Morning foot pain: Sharp discomfort often occurs with the first steps after waking.
- Getting up from a seated position: Pain may appear after standing following periods of rest.
- Extended weight-bearing activities: Walking, running, or standing for long periods can worsen discomfort.
In some cases, pain may also be felt along the arch of the foot, though this is less frequent than heel pain.
When to see a doctor
If you’re experiencing mild to moderate pain in the heel that does not resolve after a few weeks, make an appointment to see an orthopedic specialist. During the appointment, you’ll be asked to describe your pain. Your doctor will then examine your foot for tenderness and to rule out other possible causes of heel pain, such as a stress fracture or nerve entrapment syndrome. You may also need to get an X-ray to look for bone spurs. Very rarely, a magnetic resonance imaging (MRI) scan may be needed to confirm the diagnosis.
Non-operative treatment
Approximately 98.5% of plantar fasciitis cases improve with conservative care. Initial treatment options focus on reducing strain, supporting the foot, and relieving inflammation, and include:
- Silicone heel wedges, soft arches, or custom orthotics: Provide extra support and cushioning to reduce stress on the plantar fascia.
- Modifying activities: Temporarily limiting high-impact movements helps the ligament heal.
- Achilles tendon stretching: Improves calf flexibility, reducing tension on the plantar fascia.
- Plantar fascia stretching: Directly stretches and relieves stress on the inflamed ligament.
In more severe cases, immobilization and physical therapy may be recommended. If plantar fasciitis symptoms persist for several months, a cortisone injection can be administered to reduce inflammation and relieve heel pain.
Try these exercises to help address your condition:
Below is a PDF of the Exercise Program
Surgical Treatment
In rare cases, plantar fasciitis may require surgical intervention to relieve symptoms. You may need surgery if your plantar fasciitis symptoms persist for six to 12 months in spite of conservative treatment. There are two surgeries that are used for plantar fasciitis treatment. Each procedure can be performed arthroscopically (through a tiny incision) or using an open technique (through a larger incision). These procedures are:
- Plantar fascia release: A small part of the fascia is cut to release tension and therefore relieve symptoms.
- Gastrocnemius recession: A small cut is made in the gastrocnemius tendon, loosening and lengthening the muscle to release tension in the plantar fascia.
Recovery
Since plantar fasciitis treatment is usually conservative, you can quickly return to play. However, symptoms can sometimes last for months, even with appropriate conservative treatment.
If you have surgery for plantar fasciitis, recovery time will depend on whether you had open or arthroscopic surgery. Following an open plantar fascia release or gastrocnemius recession procedure, you will be required to wear a protective brace or boot for two to three weeks. Recovery will involve physical therapy, but you will not be allowed to run or jump for at least three months following the procedure. Before you can return to full athletic activities, your doctor will expect you to have regained a full range of motion and strength without any pain.
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
Which exercises should be avoided with plantar fasciitis?
Avoiding high-impact exercises, such as running or jumping, is best when dealing with plantar fasciitis. Without proper warm-ups, these activities strain your feet and ankles, leading to tight muscles and further injuries.
Can plantar fasciitis heal quickly?
It’s essential to rest and perform exercises to stretch your plantar fascia. Recovery can take a while. It may take several months or even up to a year for the pain to subside entirely.
What’s the best way to relieve plantar fasciitis pain?
One simple technique is to roll a soft-spiked plastic ball under your foot, which can be a massage. You may also be prescribed nonsteroidal anti-inflammatory drugs (NSAIDs), like naproxen or ibuprofen. These drugs will help reduce pain and inflammation over a 10—to 14-day period.
How is plantar fasciitis treated?
Most cases improve with stretching exercises, orthotics, activity modification, and sometimes physical therapy or injections.

