Osteochondritis Dissecans of the Knee Symptoms & Treatment
Osteochondritis dissecans of the knee is a joint condition in which a small segment of bone beneath the knee cartilage, the smooth, protective tissue that helps the joint move easily, loses its blood supply. This causes the bone to weaken, leading to loosening or separation of the overlying cartilage. As a result, pain, swelling, and difficulty moving the knee can develop. Osteochondritis dissecans of the knee is most commonly seen in children and adolescents, especially those who are active in sports during periods of rapid growth. Unlike sudden traumatic injuries, this condition typically develops gradually due to repetitive stress on the knee joint
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
Osteochondritis dissecans knee lesions progress through four stages. Understanding the stage helps determine the most appropriate treatment.
- Stage I The cartilage over the affected bone thickens, but both the cartilage and underlying bone remain stable. Pain is usually mild and often occurs only during activity.
- Stage II Small cracks begin to form in the cartilage surface. The bone underneath is still attached, but symptoms such as pain and swelling become more noticeable, especially after sports or physical activity.
- Stage III The cartilage is completely cracked, and the underlying bone becomes unstable. Patients may experience mechanical symptoms such as catching, locking, or a feeling that the knee is giving way.
- Stage IV The bone and cartilage fragment fully detach and become loose within the knee joint. This advanced osteochondral injury causes significant pain, swelling, and restricted motion and often requires surgical treatment.
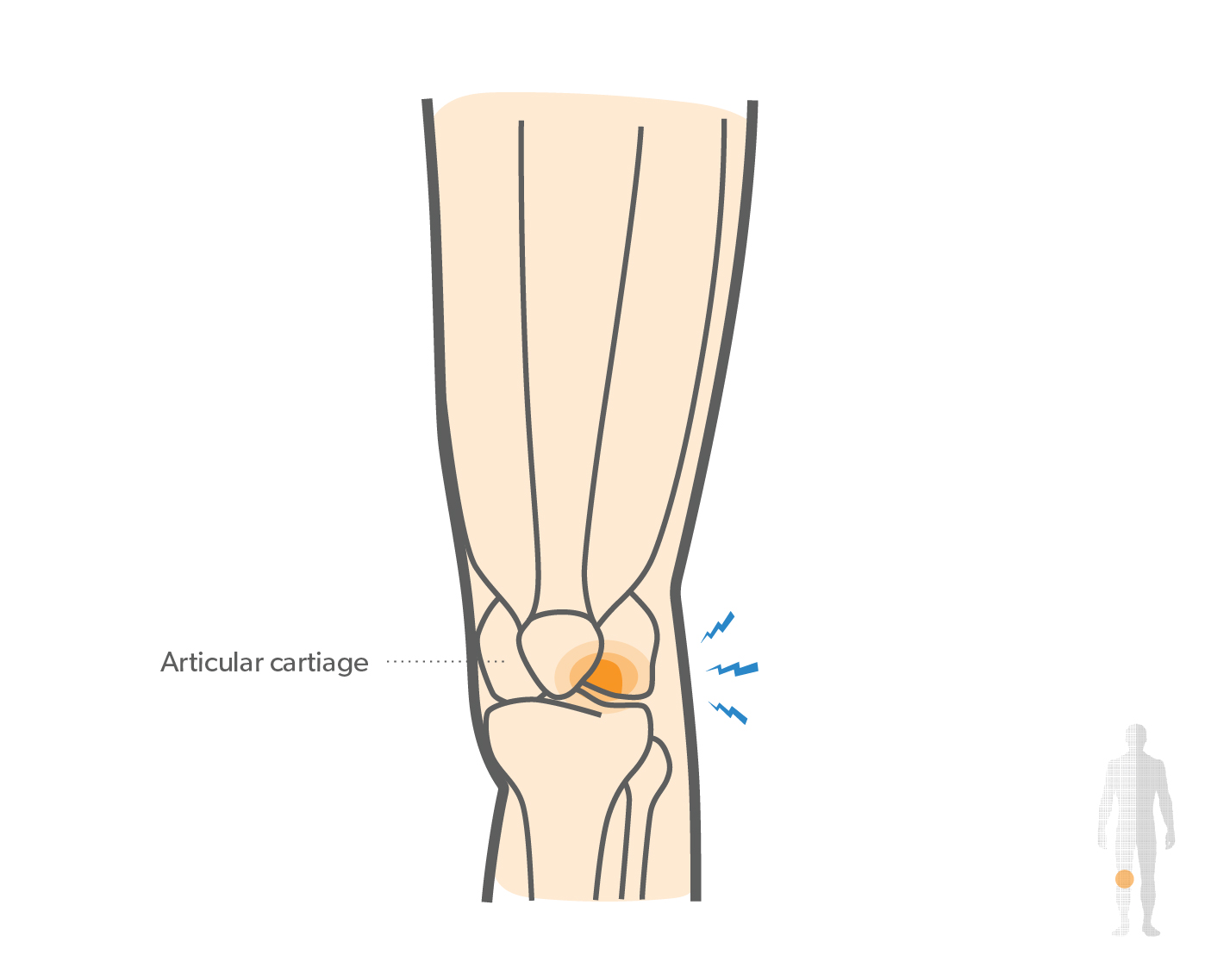
What causes Osteochondritis Dissecans of the Knee?
The exact cause of osteochondritis dissecans is not fully understood, but the condition is believed to result from disrupted blood supply to the bone beneath the cartilage.
1. How Osteochondritis Dissecans Develops
Osteochondritis dissecans in the knee develops slowly over time and in many cases the cause is not known. It is believed that repeated stress or changes in blood flow to a small area of bone may play a role. Without adequate blood supply, the bone weakens and cannot support the cartilage above it. Over time, this leads to cartilage damage and instability.
2. Causes and Risk Factors
Several factors increase the risk of developing osteochondritis dissecans knee lesions, including:
- Repetitive impact or overuse of the knee joint
- Participation in high-impact sports during growth spurts
- Poor alignment of the knee or lower limb
- Muscle imbalances that increase joint stress
- Genetic predisposition
Osteochondritis dissecans may occur with or without a specific injury and often develops silently until symptoms appear.
Sports Commonly Associated with Osteochondritis Dissecans
Certain sports place repeated stress on the knee joint and increase the risk of an osteochondral injury, including:
- Running
- Basketball
- Soccer
- Gymnastics
These activities involve frequent jumping, landing, pivoting, and repetitive loading of the knee.
Symptoms
Osteochondritis dissecans symptoms often begin gradually and worsen over time. Common symptoms include:
- Knee pain that increases with activity and improves with rest
- Mild to moderate swelling, particularly after sports
- Clicking, catching, or locking sensations during knee movement
- Decreased range of motion, making it difficult to fully bend or straighten the knee
- A feeling of instability in more advanced cases
Symptoms are typically localized to the knee and may be mistaken for general overuse injuries in the early stages.
When to see a doctor
You should see a doctor if knee pain, swelling, or stiffness persists despite rest or interferes with daily activities or sports participation. Early evaluation is essential to prevent progression to unstable disease and long-term joint damage.
Medical Evaluation
Your doctor will:
- Perform a detailed physical examination of the knee
- Order X-rays to assess bone involvement
- Use MRI to evaluate cartilage damage, determine lesion stability, and confirm the stage of osteochondritis dissecans knee disease
Early diagnosis improves treatment outcomes and reduces the risk of long-term complications.
Non-operative treatment
In children and adolescents with open growth plates, osteochondritis dissecans in the knee often heals with conservative care.
Non-operative treatment may include:
- Rest and avoidance of high-impact activities
- Temporary use of crutches to reduce weight-bearing stress
- Bracing or splinting to protect the knee
This approach focuses on allowing the bone and cartilage to heal naturally.
Rehabilitation
A structured rehabilitation program is essential for restoring knee strength, flexibility, and function. Exercises focus on:
- Improving quadriceps and hamstring strength
- Restoring normal knee motion
- Gradually returning to activity without overloading the joint
(Refer to the PDF Exercise Program below)
Osteochondritis Dissecans
Surgical Treatment
Surgery is more commonly recommended for:
- Older adolescents and adults
- Advanced or unstable osteochondral injuries
- Fully detached bone and cartilage fragments
Surgical options include:
- Fixation of loose bone fragments back into place
- Removal of detached fragments
- Techniques to stimulate new bone and cartilage growth
The goal of surgery is to restore joint surface integrity, relieve symptoms, and prevent early arthritis.
Recovery
Non-surgical Recovery
Most athletes return to activity within 2–4 months once pain, swelling, and motion limitations resolve.
Post-surgical Recovery
- Crutches are typically required for approximately 6 weeks
- Physical therapy follows to restore strength and motion
- Full recovery may take 3–6 months, depending on lesion severity and treatment type
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
Is osteochondritis dissecans caused by a sudden injury?
No. Osteochondritis dissecans in the knee usually develops gradually due to repetitive stress rather than a single traumatic event.
Will osteochondritis dissecans heal without surgery?
In many children and adolescents, the condition heals with rest, activity modification, and monitoring.
What happens if osteochondritis dissecans is left untreated?
Untreated disease can progress to unstable lesions, loose fragments, chronic pain, and early-onset knee arthritis.
How long does it take to return to sports after OCD of the knee?
Return to sports typically ranges from 2 to 6 months, depending on healing, symptom resolution, and whether surgery was required.

