Carpometacarpal (CMC) Arthritis Symptoms & Treatment
The carpometacarpal (CMC) joint, also called the basal joint, connects the base of your thumb to your wrist. This joint plays a major role in pinching, gripping, and overall thumb movement. Carpometacarpal arthritis develops when the cartilage in this joint wears down over time, leading to thumb joint pain, stiffness, and reduced thumb function. As the condition progresses, simple daily activities—such as opening jars, turning doorknobs, or holding objects—can become painful and difficult.
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
The carpometacarpal joint of the thumb is one of the most flexible joints in the hand. Unlike the other carpometacarpal joints, the thumb CMC joint allows motion in multiple directions, including pinching and grasping. Because of this frequent use, the joint is more vulnerable to wear and tear. When arthritis affects this joint, pain and loss of motion can significantly impact hand strength and daily function.
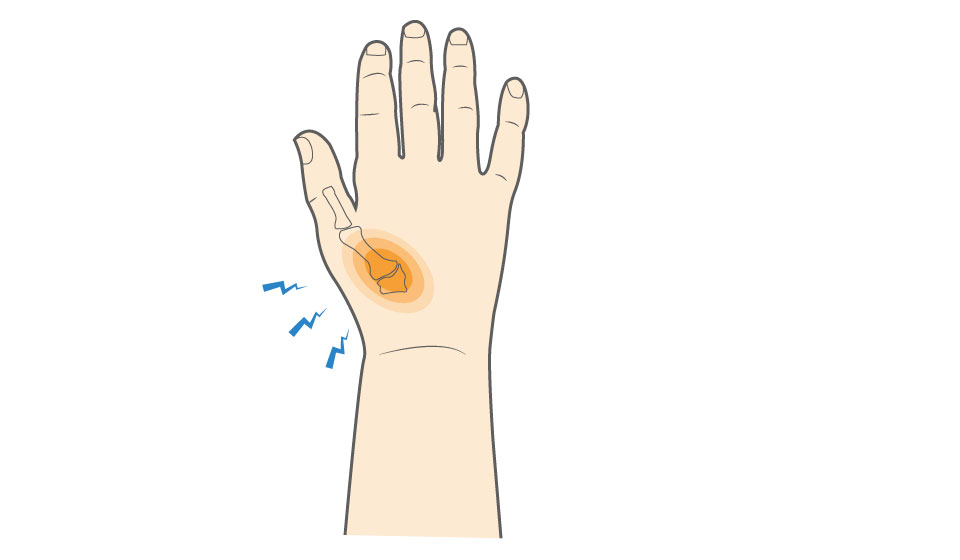
What causes Carpometacarpal (CMC) Arthritis?
Carpometacarpal arthritis most often occurs due to osteoarthritis, a condition where the smooth cartilage that cushions the joint gradually breaks down. As the cartilage wears away, the bones in the joint begin to rub against each other. This friction causes irritation, inflammation, swelling, and increasing pain at the base of the thumb.
Over time, this damage leads to stiffness and reduced range of motion, making it harder to use the thumb without discomfort.
How the Condition Develops
CMC arthritis usually develops slowly over many years. Repeated stress on the thumb joint, combined with natural aging, can weaken the cartilage. As the joint loses its protective cushioning, everyday movements place more strain on the bones, worsening thumb pain and limiting hand function.
Common Everyday Risk Factors
Several factors can increase your risk of developing carpometacarpal arthritis, including:
- Being female, as women are more likely to develop CMC arthritis
- Age over 40, when cartilage naturally begins to thin
- Genetic factors, such as joint shape abnormalities
- Inflammatory conditions, including rheumatoid arthritis
- Previous thumb injuries, such as fractures or sprains
In some cases, arthritis develops years after an injury. This is known as post-traumatic arthritis.
Sports Linked to Thumb Injuries and Post-Traumatic CMC Arthritis
Certain sports increase the risk of thumb injuries that may later lead to carpometacarpal arthritis:
- Skiing – Falls often cause the thumb to twist forcefully
- Baseball – Repeated gripping and impact from catching
- Volleyball & Basketball – Jamming the thumb during play
- Football, Hockey, and Rugby – High-contact collisions stress the thumb joint
These activities place repeated force on the carpometacarpal joint of the thumb, increasing the chance of long-term joint damage.
Symptoms
The most common symptom is pain at the base of the thumb, especially during gripping or pinching. Other symptoms may include:
- Stiffness and swelling around the thumb joint
- Tenderness at the base of the thumb
- Reduced thumb movement and flexibility
- Weakness when pinching or holding objects
- A visible joint deformity as the arthritis worsens
As the condition progresses, symptoms may occur even at rest.
When to see a doctor
You should see a doctor if you have ongoing thumb pain, swelling, or stiffness that does not improve or begins to interfere with daily activities. Early diagnosis can help slow progression and preserve hand function.
During the exam, your doctor will assess swelling, tenderness, and range of motion. They may move your thumb while holding the CMC joint to check for pain, grinding, or a gritty sensation—signs that cartilage has worn down. X-rays may be ordered to look for joint space narrowing, bone spurs, or other signs of carpometacarpal arthritis.
Non-operative treatment
Early-stage CMC arthritis is often managed without surgery. Treatment focuses on reducing inflammation and relieving pain, and may include:
- Avoiding activities that worsen thumb pain
- Using topical pain-relief medications
- Taking NSAIDs such as ibuprofen or naproxen
- Wearing a thumb splint to limit movement and reduce stress
- Corticosteroid injections to decrease inflammation
Your doctor may also recommend hand exercises to maintain strength and flexibility. A guided exercise program can help support the carpometacarpal joints and reduce stiffness.
Try these exercises to help address your condition:
Below is a PDF of the exercise program.
Surgical Treatment
If symptoms become severe or non-operative treatments no longer help, surgery may be recommended. Surgical options include:
- CMC joint fusion, which permanently joins the bones to eliminate painful movement
- Osteotomy, where bones are repositioned to improve alignment
- Trapeziectomy, which removes the trapezium bone to create more space in the joint
- Joint replacement (CMC arthroplasty), replacing the joint with a tendon graft
Most CMC arthritis surgeries are outpatient procedures, allowing patients to return home the same day.
Recovery
Carpometacarpal arthritis is a chronic condition, meaning symptoms may flare up over time. Lifestyle adjustments, adaptive tools, and hot or cold therapy can help manage discomfort.
After surgery, patients usually wear a cast for 3–4 weeks, followed by a splint for several more weeks. Regaining thumb motion typically takes 6–8 weeks, while full recovery may take several months. Hand therapy plays an important role in restoring strength and flexibility.
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
What are the common signs of CMC arthritis?
Pain at the base of the thumb, swelling, stiffness, weakness, and difficulty pinching or gripping objects.
Who is most likely to develop CMC arthritis?
Women, adults over 40, people with joint injuries, and those with inflammatory conditions are at higher risk.
How is CMC arthritis usually treated?
Treatment often starts with splinting, medications, and therapy. Surgery is considered if symptoms become severe.
Can I stay active with CMC arthritis?
Yes. With proper treatment and activity modification, many people remain active while managing symptoms.

