Avascular Necrosis (AVN) Causes, Symptoms & Treatment
Avascular Necrosis (AVN) is a condition where reduced blood flow to a bone leads to the death of bone tissue. It most often affects the hip but can occur in other joints. As the bone weakens, pain, stiffness, and limited movement develop. Early diagnosis and treatment are important to prevent joint collapse and long-term disability.
Start with our quick Symptom Assessment or connect directly with an Upswing Coach today.
Request an AppointmentReady to take the next step?
Start your symptom assessment or connect with a coach instantly.
Find Relief TodayOverview
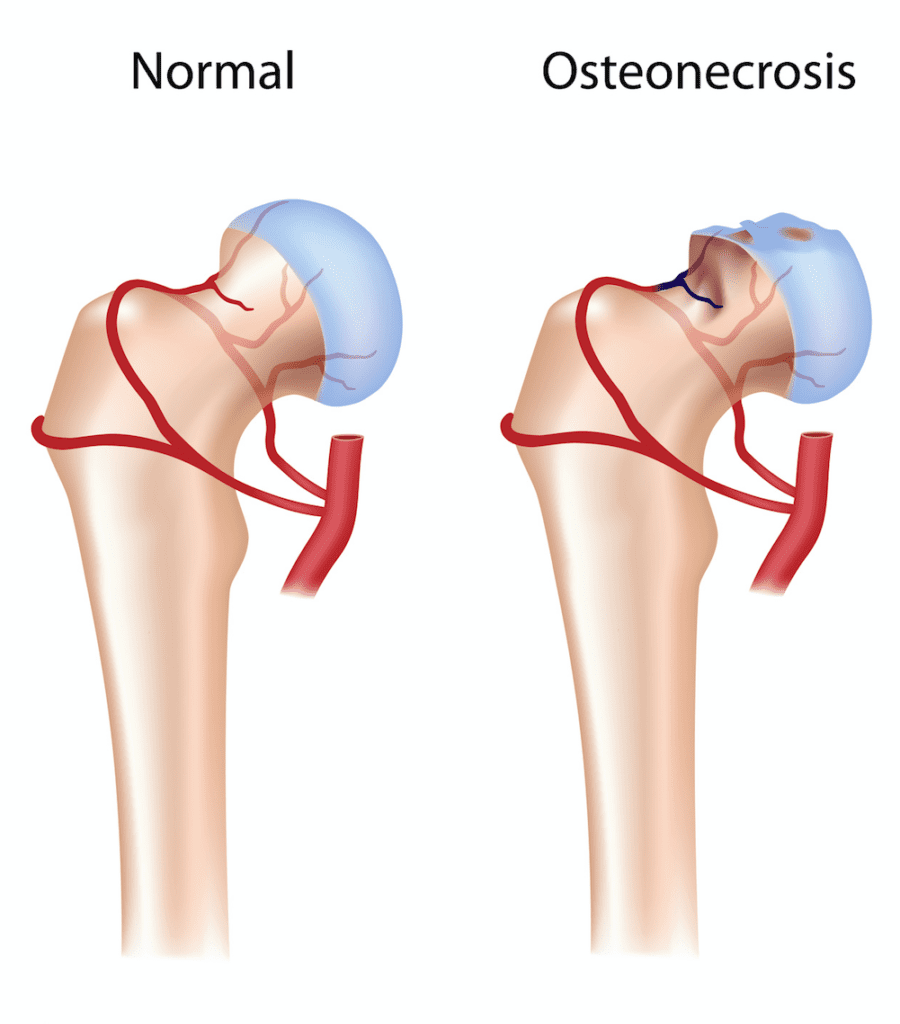
The hip works as a “ball and socket” joint, where the ball at the top of the femur fits into the acetabulum(socket) of the pelvis. Sometimes the femoral head loses its blood supply, and much like a heart attack affecting the heart muscle, the bone begins to die. This is known as Avascular Necrosis (AVN) of the femoral head (or osteonecrosis). About 20,000 new cases are identified each year.
The condition is painful, and without proper treatment, the femoral head may collapse and lead to dysfunction of the entire hip joint.
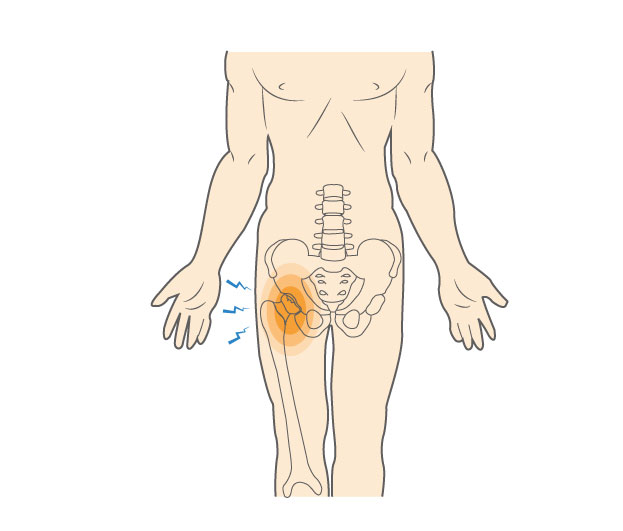
What causes Avascular Necrosis (AVN)?
Bones rely on a steady blood supply to remain strong. When circulation to the femoral head is interrupted, the bone weakens and eventually dies. A major hip injury, such as a dislocation or fracture, can trigger AVN by damaging the blood vessels that support the bone.
High-impact collision sports increase the risk of this type of trauma. Other contributing factors include heavy alcohol use, long-term corticosteroid therapy, and certain medical conditions such as sickle cell disease or Crohn’s disease.
- How the Injury Occurs: AVN develops when a significant injury or an internal condition restricts blood flow to the femoral head, causing the bone to deteriorate over time. Without adequate blood supply, the bone tissue collapses, and the hip joint begins to fail.
- Common Everyday Causes: Outside of sports, AVN may result from long-term steroid use, heavy alcohol consumption, or medical conditions that affect circulation. In some cases, a fall, a car accident, or the cumulative effects of certain medications can disrupt blood flow and lead to this condition.Sometimes the cause is never determined.
Sports Where AVN of the Hip Is Most Common:
- Soccer: Hard tackles and sudden collisions can cause traumatic hip injuries.
- Football: High-impact hits increase the likelihood of hip dislocations and fractures.
- Basketball: Intense jumping and fast contact play can stress or injure the hip.
- Rugby: Frequent heavy collisions place athletes at risk for severe hip trauma.
Volleyball: High-energy landings and unexpected falls can affect hip stability.
Symptoms
Avascular Necrosis often develops slowly, and early in the condition, athletes may not notice any changes. As it progresses, hip pain becomes more noticeable, especially during activity. Common symptoms include:
- Constant hip pain that may continue even during rest
- Pain that spreads to the groin, thigh, or buttocks
- Difficulty walking without a limp or shifting weight to the healthy leg
- Stiffness and a reduced range of motion in the hip, which makes bending or turning uncomfortable
When to see a doctor
Athletes should see a doctor if they develop hip pain after a serious fall or major trauma, especially if the discomfort does not improve.You should also see your doctor if you have hip pain without an injury that does not improve over time. During the evaluation, the doctor may ask you to move your hip in different directions to assess pain, stiffness, and range of motion. In the early stages of AVN, symptoms may be mild, and hip movement may seem normal. Providing details about your injury history, medical conditions, and lifestyle habits is important for an accurate diagnosis.
Your doctor may order an X-ray and, if AVN is suspected, an MRI. X-rays often show bone damage only in later stages, while MRI scans can detect early changes in the femoral head. This helps identify AVN before significant structural damage develops.
Non-operative treatment
When AVN is detected early, conservative treatment can help ease pain and may slow or even stop the condition from progressing. Non-surgical options your doctor may recommend include:
- Rest, to reduce stress on the hip joint
- Using crutches and limiting weight-bearing for up to six weeks to protect the femoral head
- Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen are used to manage pain and inflammation
- Gentle exercises, such as riding a stationary bike or walking in a pool, to maintain mobility without
Try these exercises to help address your condition:
Below is a PDF of the Exercise Program
Surgical Treatment
For many patients with AVN, surgery is the most effective option. If the condition is detected early, before the femoral head collapses, certain procedures may help preserve the hip. Core decompression involves drilling into the affected bone to stimulate new blood vessel growth and replace dead bone with healthy tissue. Other options include bone grafts, which use healthy bone from another part of the body or a donor.
When AVN advances and the femoral head collapses, a total hip replacement may be necessary. This procedure removes the damaged joint and replaces it with an artificial ball-and-socket joint.
Recovery
Recovery outcomes depend on the procedure performed and the stage of AVN. Core decompression is most effective when done early, while total hip replacement typically provides excellent pain relief and restores joint function. Recovery can take several months and usually includes a structured physical therapy program.
Factors such as age, overall fitness, and the intensity of athletic activity affect how quickly an athlete can return to full or modified participation. Doctors guide patients throughout the rehabilitation process to ensure a safe and effective recovery.
Dr. Jay Kimmel is a board-certified orthopedic surgeon specializing in sports medicine, arthroscopic surgery, and shoulder and knee disorders. He completed his orthopedic training at New York-Presbyterian/Columbia University Medical Center and a Sports Medicine Fellowship at Temple University.
Dr. Kimmel previously served as the Director of the Connecticut Sports Medicine Institute at Saint Francis Hospital and has held faculty appointments as Clinical Assistant Professor in the Departments of Orthopedics and Family Medicine at the University of Connecticut. He has extensive experience caring for athletes as a team physician for high school and collegiate programs and continues to teach in the athletic training departments at Westfield State University and Springfield College.
Find the Support You Need — Right When You Need It
Whether you’re managing pain for the first time, need ongoing guidance, or require expert medical care, we’re here to help you every step of the way.
ORTHO DIRECT
Video visit with an orthopedic doctor for advice and a care plan.
$30
/MonthMRI DIRECT
Fast, affordable MRI with orthopedic review. No insurance required.
$499
/MonthFrequently Asked Questions
Is surgery always required for AVN?
Not always. Many early-stage cases improve with non-surgical treatments such as rest, medication, and gentle exercises.
Can athletes return to sports after AVN treatment?
Yes. With proper care and rehabilitation, most athletes regain function and can return to full or modified activity.
Does hip replacement improve quality of life?
Yes. Total hip replacement can relieve pain, restore mobility, and allow patients to comfortably resume daily and athletic activities.
Can AVN be prevented from worsening?
Early diagnosis, avoiding further trauma, and following your doctor’s treatment plan can help protect the hip and prevent progression

